The 21st Century CURES act has mandated that starting on April 5th, 2021 patient notes (with a few very narrow exceptions) must be easily available to patients via their patient portal. How did this come about, and what does it mean for us?
In this Vodcast episode. Dr. Andrew Fried, ultrasound Jedi, give us a masterclass on placing ultrasound guided IVs.
This year we are very fortunate to have Dr. Amal Mattu, EKG Jedi, as teaching faculty for our 39th Maine Medical Center/Maine ACEP Winter Symposium. In this lecture, he helps us differentiate septal STEMIs from other potentially life threatening mimics.
Ludwig’s Angina is an uncommon but dangerous floor of the mouth infection. It is important to recognize and manage it appropriately. For this reason we present images and video of a case of Ludwig’s Angina… and sprinkle in nuggets of wisdom regarding source, presentation, complications, and management.
In this post and podcast we review mRNA vaccines and the Pfizer phase 3 study to help frontline providers answer some important questions- What is an mRNA vaccine? How does this differ from the traditional vaccines? Is it safe? Efficacious? We take a closer look at the recent NEJM article to help us come to a final answer on the most important question- Should I feel comfortable getting this vaccine?
Intubation in the emergency department (ED) can be a stressful endeavor. We are often presented with patients who have complex anatomy and tenuous physiology. Because of this, it can be hard to look past the critical step of securing the airway. Rapid sequence intubation (RSI) and positive pressure ventilation can dismantle patients’ physiology and contribute to an almost 4% rate of post intubation cardiac arrest (PICA). Is there anything we can do to predict or prevent this? In this podcast, Sam Wood gives us an overview of the literature to help us answer these questions.
The management of diabetic ketoacidosis (DKA) in children is full of difficult questions- how much insulin should I give? Who is at risk for cerebral edema? What treatments, if any, increase the risk for this dreaded complication? Which fluid is ideal? How much of this fluid should I give? We sat down with ED physician and endocrine aficionado Dr. George Willis to answer these questions.
They have something DOWN THERE... No surprises, it's herpes. But making the diagnosis is the just first of many issues and questions- how do you treat it? Will it come back? How do I stop from spreading it to other partners? Is there something I can do to decrease my number of outbreaks? All great questions we should be ready to answer. In this vodcast Dr. Leger reviews this disease and these important questions.
The diagnosis of Wernicke's encephalopathy is an elusive beast. The classic triad of altered mental status, ataxia, and ophthalmoplegia is, of course, anything but classic in terms of presentation. To make matters worse, the most at-risk population, the chronic alcohol misuser, often have these signs and symptoms for alternative reasons. In this podcast we discuss diagnosing Wernicke's in the alcoholic.
Emergency physicians regularly see psychiatric patients who are having suicidal thoughts or engage in non-suicidal self-injurious (NSSI) behavior. In addition to working these patients up medically, it is part of our job to determine who needs emergent evaluation by a psychiatric provider and who is safe for discharge. This is a very important decision, as we do not want to send high risk patients home and keep low risk patients for extended periods of time while they await their evaluation. Balancing this can be difficult - oftentimes it is not obvious where a patient falls on this spectrum. We are taught various decision aids in medical school to help us risk stratify these patients - but how do they perform on emergency department patients? For this month's journal club, we looked at three papers that examine three different decision aids to help elucidate this issue.
Urinary complaints in females are an incredibly common reason for visits to emergency departments. We are often left to make the decision of whether to treat for infection on fairly equivocal urinalysis results without the help of a definitive culture. Muddying the waters is the risk of sexually transmitted infections (STI's) which can cause similar if not more benign symptomatology (even at times completely asymptomatic). Can the history help? Do reported symptoms correlate with a diagnosis? In April's journal club, we chose articles that aimed to clarify the distinction between two entities (UTI vs. STI) that are incredibly frequent in sexually active women.
The availability of herbal and dietary supplements in the U.S. is increasing exponentially: 4,000 in 1994 to 80,000 today. Half of all adults have reported using at least one dietary supplement in the past month, but many do not openly relay this to their primary care physicians or emergency medicine physicians. This month’s journal club focused on the utilization of these products, their adverse events/complications as well as their “regulation”.
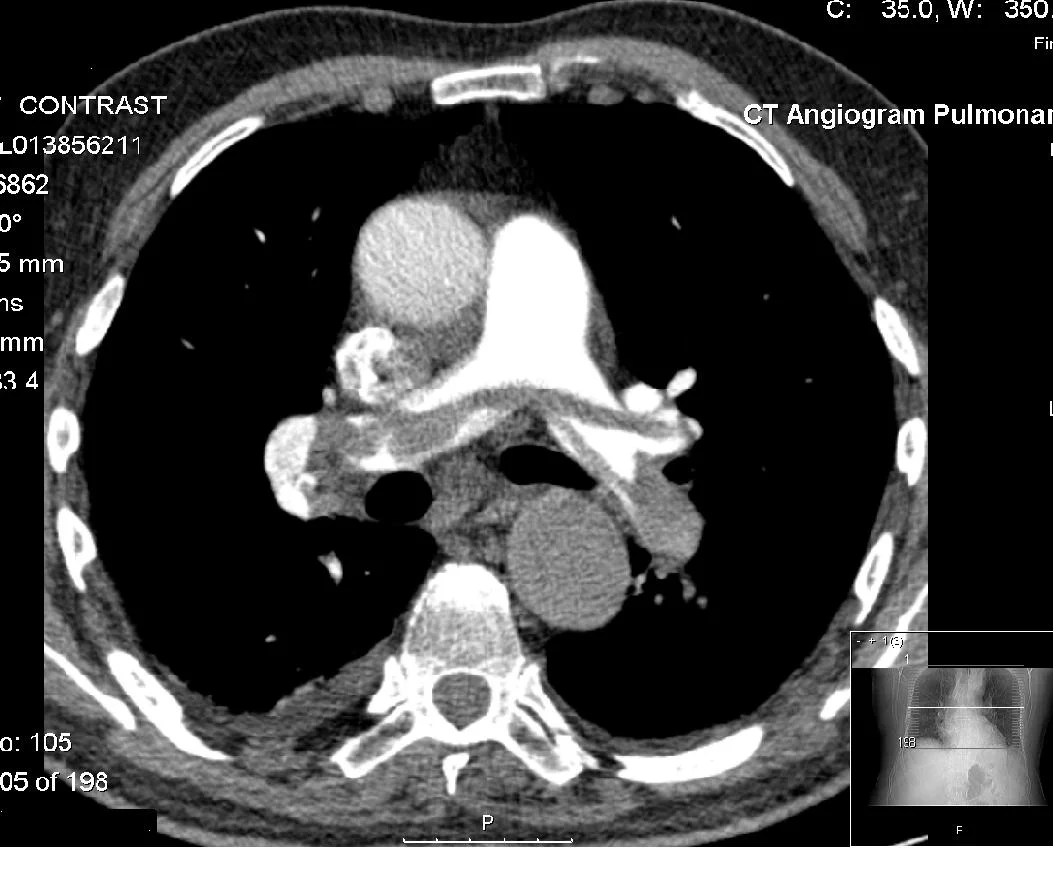
Since Prandoni et al published their findings in the NEJM's October 2016 issue (reporting a 17.3% incidence of pulmonary embolism among patients admitted with first time syncope), there has been controversy swirling in the EM community. Questions have been raised regarding the impact of this study, its generalizability, and its implications for clinical practice. At this month’s journal club, we broke down the findings in the Prandoni study as well as looked at two other studies (Castelli et al and Altinsoy et al) that examined the clinical characteristics of patients with PE who presented with syncope.
At this journal club we looked at a number of studies examining the concept. While they were of varied design, the premise of all was the same; namely with an antibiotic only approach, what is the success rate, recurrence rate, and cost savings / loss?
This month Dr. Rappold opened up his home to us where we discussed the utility of bedside ultrasound and plain films in the resuscitation of the trauma patient.

























Interviewing and beginning your career in medicine comes with challenges! Dr. Sarah Bunting, MD is a PGY-1 emergency medicine resident at Maine Medical Center. Listen in to hear her advice on transitioning from medical school to residency, virtual interviewing, and what to look for in a residency!